Know Ortho: Managing the Fragility Hip Fracture on the USMLE
- by
- Aug 14, 2018
- Reviewed by: Amy Rontal, MD
Hip fractures in the elderly are common, with a prevalence of 0.2% in men and 0.5% in women, which means you can expect to see a question or two on the USMLE. Not only does this condition encompass orthopaedic surgical management of a very common fracture, but it also serves to review medical management of a fragile patient who is at risk for a fracture through osteoporotic bone. In a nutshell, an insufficiency or fragility fracture of the hip occurs when a person falls onto an osteoporotic hip. Patients often present with anterior thigh or groin pain, a shortened and externally rotated lower extremity (the adductors shorten, gluteus medius and maximus abduct, iliopsoas flexes, and the short external rotators, you guessed it, externally rotate), and inability to ambulate.
When encountered with this individual, it is important to understand not just the fracture, but also why the person fell! Causes of fall are numerous and can have cardiac, neurologic, hematologic, and endocrine etiologies among others; it is up to you to elucidate this. I cannot stress the importance of working up the patient for an etiology of the fall. Remember, the treatment of these fractures is often surgical and we need to ensure the patient is medically capable of undergoing a rather extensive operation and receiving an anesthetic. Standard workup of these patients includes basic labs complete blood count and serum chemistries – chest x-ray to evaluate for things like pneumonia, and electrocardiogram to evaluate for conditions like arrhythmia and myocardial infarction. Other diagnostic modalities including non-contrasted CT of head to look for hemorrhagic stroke and echocardiogram to evaluate for motion or valvular abnormalities should be considered in the appropriate setting. That said, it is always possible that the individual suffered a mechanical fall from tripping on loose rugs or dog toys, and you may not find an abnormality on your workup! Once you’ve found an abnormality, you should aim to optimize it for surgery i.e. replete electrolytes, rate or rhythm control an arrhythmia, resuscitate a hypovolemic patient, etc. As soon as the patient is optimized, you can hand the patient off to the orthopaedic surgeon for fracture management.
The hip is a broad term. Patients may liken the hip to include the pelvis, acetabulum (socket of the hip joint), femoral head (ball of the hip joint), femoral neck, and proximal femur including the peritrochanteric region (think greater and lesser trochanters) (Figure 1).
Figure 1. Normal Anatomy of the Hip
Image Credit: Hip Fractures Diseases & Conditions
For the purpose of USMLE exams, you should familiarize yourself with fractures of the femoral neck and peritrochanteric region, as the surgical management is quite different between the two.
Let’s start with a little anatomy. The hip joint capsule extends to approximately the distal one-third of the femoral neck, encompassing the subcapital (beneath the head) and transcervical (mid neck) regions (don’t memorize this for exams, for the purpose of the USMLE just think of a femoral neck fracture as intracapsular). The femoral head is supplied predominately by the deep branch of the medial circumflex femoral artery which supplies the head in retrograde fashion by coursing around the piriformis fossa to enter the hip capsule (Figure 2).
Figure 2. Vascular Supply to the Femoral Head
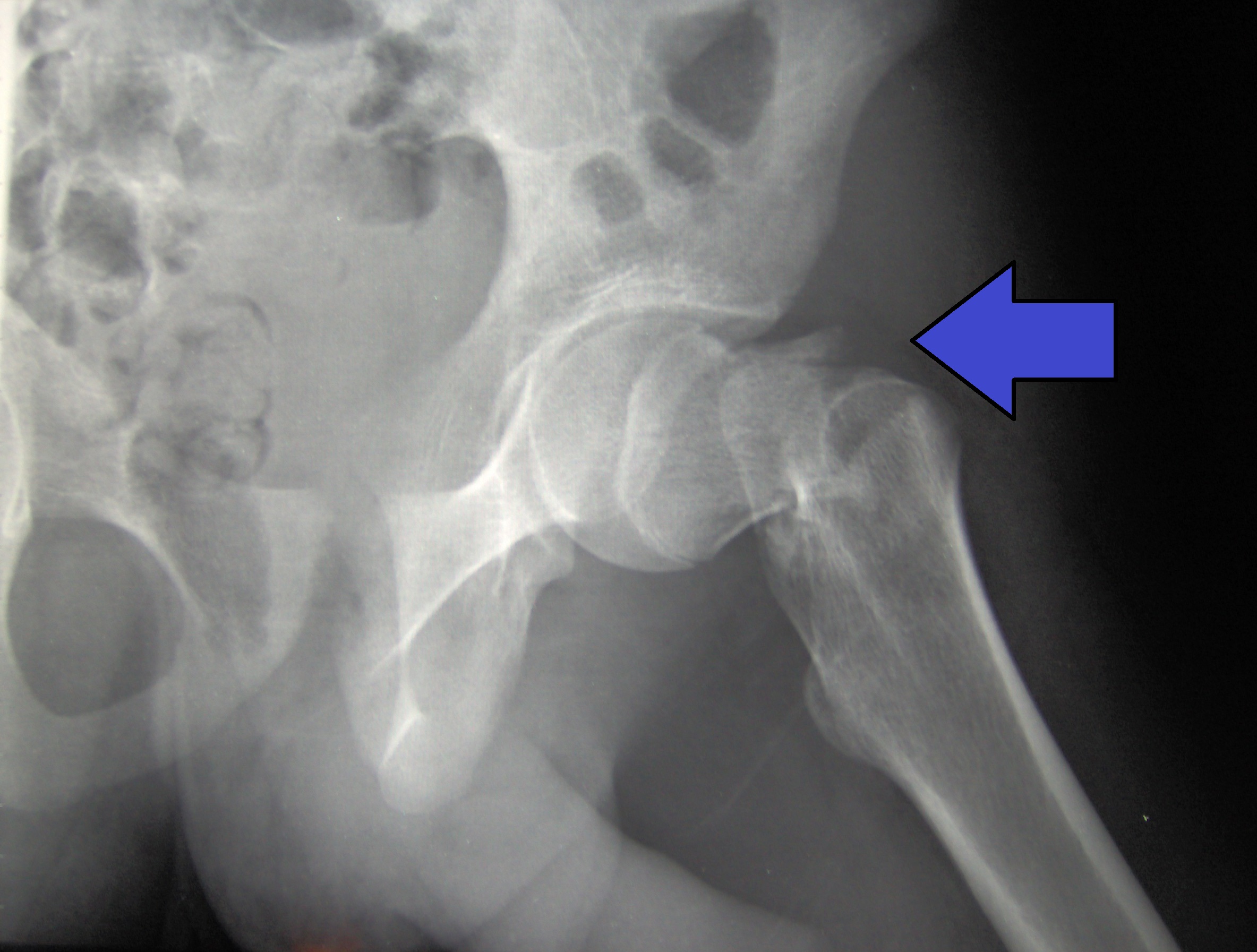
Intracapsular femoral neck fractures (specifically subcapital and transcervical, but not basicervical for you budding orthopods) place the blood supply to the femoral head at risk and may also cause a rise in intracapsular pressure that tamponades arterial flow, resulting in osteonecrosis of the femoral head (Figure 3).
Figure 3. Displaced Transcervical Femoral Neck Fracture
What does this mean? In a nutshell, displaced intracapsular fractures through the femoral neck render the femoral head at risk for osteonecrosis. If you try to fix these, your fixation may fail, the femoral head may collapse, and you can end up with an unhappy patient with pain and limited mobility. Thus, we replace displaced femoral neck fractures! Depending on your patient, you may opt to replace just the femoral side with a partial hip replacement (hemiarthroplasty) or opt to replace both the femoral side and acetabular side with a total hip arthroplasty (Figure 4).
Figure 4. Intertrochanteric Femur Fracture
For you budding orthopods, hemiarthroplasty is preferred for low demand patients with minimal pre-existing arthritis and total hip arthroplasty is preferred for high demand patients or those with arthritic changes. With both hemiarthroplasty and total hip arthroplasty, your patient can ambulate immediately.
Although termed as a hip fracture, peritrochanteric fractures, including intertrochanteric and subtrochanteric fractures, are much different from femoral neck fractures. Unlike in femoral neck fractures, the femoral head is not at risk for osteonecrosis with peritrochanteric fractures, as the fracture is extracapsular and far removed from the deep branch of the medial circumflex femoral artery (Figure 5).
Figure 5. Schematic of Hemiarthroplasty (left) and Total Hip Arthroplasty (Right)
So, management is aimed at creating a strong construct that allows for immediate mobility and restores length, alignment, and rotation. Multiple constructs have been developed to accomplish this task, the majority of which have an intramedullary nail or laterally based plate and a large cephalad screw (think directed into the femoral head). You may see cephalomedullary nail (Figure 6) (cephalad screw, intramedullary load sharing device), sliding or dynamic hip screw (Figure 7) (lateral plate with cephalad screw), or simply open reduction internal fixation to describe this.
Figure 6. Subtrochanteric Femur Fracture Treated with Cephalomedullary Implant
Figure 7. Intertrochanteric Femur Fracture treated with Sliding Hip Screw
Why are we so concerned with hip fractures? Well, the expeditious and thorough management of a patient with a fragility hip fracture can be life-saving. Without treatment, patients may develop an aspiration pneumonia, deep venous thrombosis, urinary tract infection, and pressure ulcers from remaining immobile for extended periods. You should aim to operate on these patients within 24-72 hours so that we can mobilize these patients and prevent catastrophic complications.
The next time you see a hip fracture, workup the etiology of the fall, medically optimize the patient, and refer to the orthopaedic surgeon to replace femoral neck fractures and fix peritrochanteric fractures.









